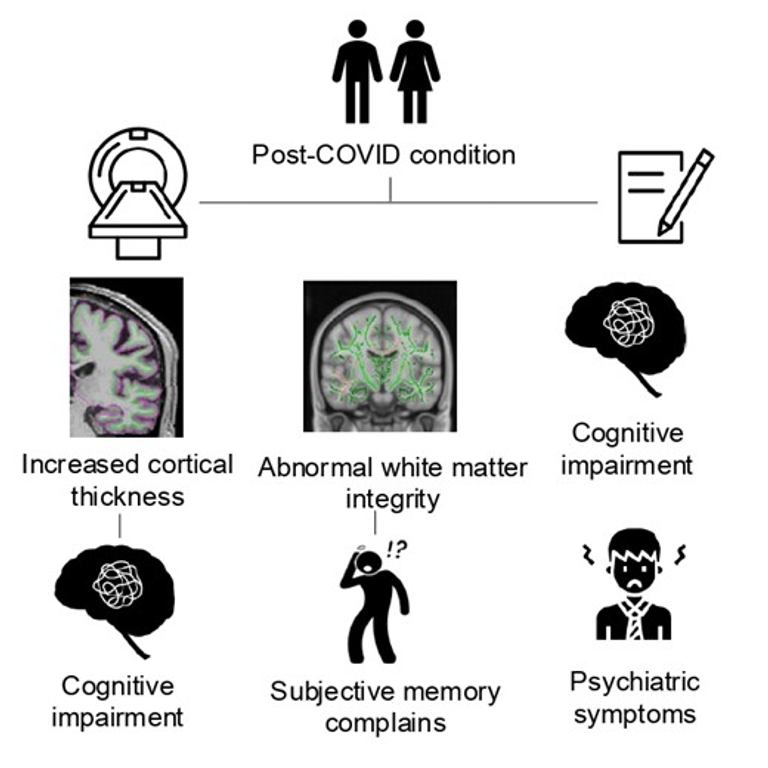
It has been estimated that approximately 4% of individuals infected with SARS-CoV-2 will be diagnosed with post-COVID condition. Previous studies have evidenced the presence of cognitive dysfunction and structural brain changes in infected individuals; however, the relationship between structural changes and cognitive alterations in post-COVID condition is still not clear. Consequently, the aim of this work is to study structural brain alterations in post-COVID condition patients after almost two years of infection and their likely relationship with patients’ cognitive impairment. Additionally, the association with blood biomarkers and clinical variables was also explored.
One hundred twenty-eight individuals with post-COVID condition and 37 non-infected healthy controls from the Nautilus Project (ClinicalTrials.gov IDs: NCT05307549 and NCT05307575) underwent structural brain magnetic resonance imaging and a comprehensive neuropsychological assessment. A subsample of 135 post-COVID participants also underwent blood extraction to obtain levels of blood biomarkers. Cortical thickness and subcortical volumes were obtained and analyzed using FreeSurfer (v7.1). FMRIB Software Library software (v6.0.4) was used to perform gray matter voxel-based analysis and to study microstructural white matter integrity.
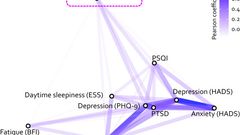
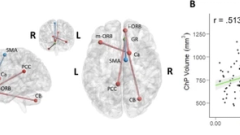
Patients with post-COVID performed significantly worse in working and verbal memory, processing speed, verbal fluency and executive functions, compared to healthy controls. Moreover, patients with post-COVID showed increased cortical thickness in the right superior frontal and the right rostral middle frontal gyri that negatively correlated with working memory performance. Diffusion tensor imaging data showed lower fractional anisotropy in patients in the right superior longitudinal fasciculus, the splenium and genu of the corpus callosum, the right uncinate fasciculus and the forceps major, that negatively correlated with subjective memory failures. No differences in blood biomarkers were found. Once patients were classified according to their cognitive status, only those post-COVID clinically cognitively altered presented increased cortical thickness compared to controls.
In conclusion, our study showed that gray and white matter brain changes are relevant in this condition after almost two years of infection and partly explain long term cognitive sequelae.
These findings underscore the critical importance of monitoring this at-risk population over time.
![Metabolic brain changes in post-acute COVID-19: systematic review and meta-analysis of [18F]-FDG-PET findings](/_vercel/image?url=%2Ftcl-fallback-169.jpg&w=320&q=100)